Publications
Harnessing the Potential of Cell Fate Reprogramming for Cancer Immunotherapy
Abstract
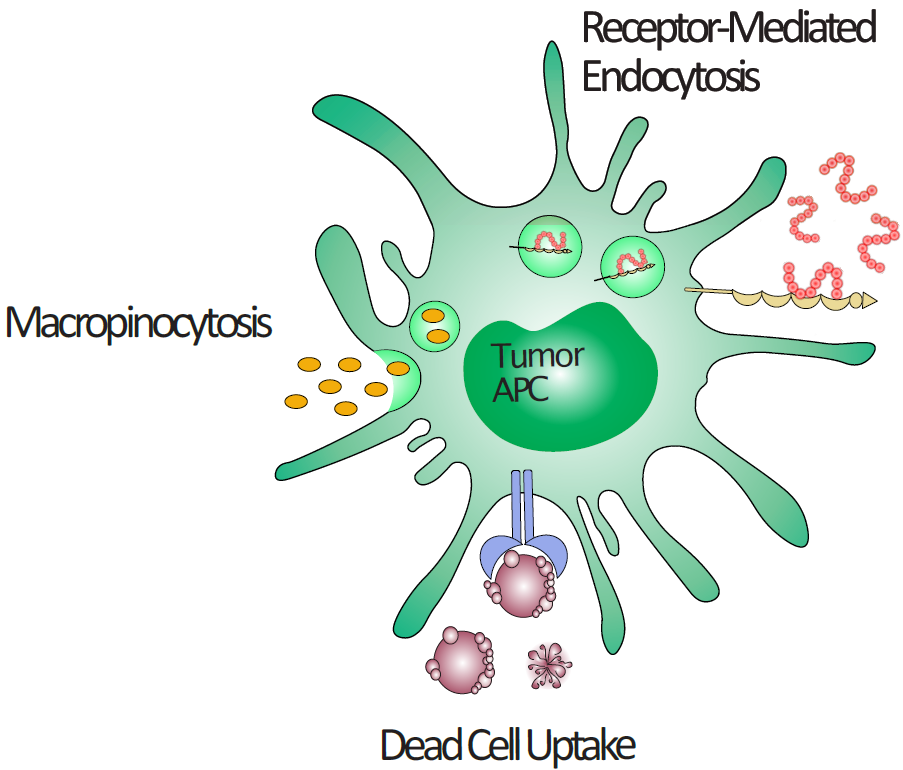
Despite significant advances in cancer immunotherapy, the majority of patients still do not benefit from treatment. Recent research has highlighted the potency of the dendritic cell subtype cDC1 to prime naïve CD8+ T cells by cross-presentation of tumor specific antigens and direct anti-cancer immunity. However, the dynamic process of immunoediting renders the cancer cells invisible for T cell recognition. Direct cell reprogramming offers the opportunity to resolve these challenges. Our group demonstrated that transcription factors Pu.1, Irf8 and Batf3 (PIB) convert fibroblasts into induced dendritic cells imposing a cDC1-like transcriptional program and cross-presentation capacity. In this study, I evaluate the transcription factor combination to reprogram murine cancer cells into professional tumor antigen presenting cells (tumor-APCs), a process conceptualized as functional reprogramming. Combined expression of PIB in melanoma and lung carcinoma induces hematopoietic and DC markers, CD45 and MHC-II, while upregulating MHC-I and costimulatory molecules CD80/86 and CD40. Notably, epigenetic modification by histone deacetylase inhibitor VPA improves reprogramming efficiency and accelerates the acquisition of a tumor-APC phenotype. Reprogramming successfully endows tumor-APCs with professional APC functions including exogenous antigen uptake by receptor-mediated endocytosis, phagocytosis or macropinocytosis, antigen processing capacity by lysosomal proteases and cross-presentation. Most importantly, PIB expression rescues self-antigen presentation leading to naive CD8+ T cell priming and exposes cancer cells to T cell mediated killing. Collectively, this study lays the foundation for further transcriptional, phenotypical and functional characterization of tumor-APCs, which will pave the way for the development of an immunotherapeutic gene therapy based on the concept of functional reprogramming.